Medicare Advantage Organizations applying for Initial Approval or Service Area Expansion (SAE) can use Letters of Intent in place of signed contracts to satisfy network adequacy requirements during the application process. This method helps applicants achieve the necessary network adequacy thresholds while finalizing contract details for expanding into new markets.
Notification Requirement: As part of the network adequacy review process, applicants must notify CMS of their use of each Letter of Intent to meet network standards. In this FAQ, we address common questions related to the use of Letters of Intent by Medicare Advantage Organizations during the application process.
Key Updates Effective January 19, 2026
New Attestation: Applicants must attest to using a Letter of Intent in their application and indicate this on their Health Services Delivery (HSD) table in the initial submission.
Elimination of PDF Upload: Applicants are not required to upload the PDF Letter of Intent with their HSD tables.
Discontinuation of LOI Matrix Form: There is no longer a need to complete a Letter of Intent Matrix form.
Letter of Intent During the Application Process
Q: Why do Medicare Advantage Organizations use Letters of Intent during the application process?
A: Letters of Intent allow Medicare Advantage Organizations to meet network adequacy requirements while applying for initial approval or service area expansion. Building an adequate network before receiving a Medicare Advantage contract can be challenging. Letters of Intent serve as placeholders for signed contracts during this period.
Q: When can you use a Letter of Intent to demonstrate network adequacy?
A: You can use a Letter of Intent in the following scenarios:
- For Initial Approval counties
- For Service Area Expansion counties
Q: Can Letters of Intent be used with active counties?
A: No, Letters of Intent can only be used for Initial Approval or Service Area Expansion counties.
Q: When can applicants include Letters of Intent in their network adequacy submissions?
A: Applicants can include Letters of Intent during the following submissions:
- Initial Submission
- In response to a Deficiency Notice
- In response to a Notice of Intent to Deny
Q: How do applicants include Letters of Intent in their Initial Network Submission?
A: Applicants should:
- Include providers and facilities with valid Letters of Intent in the initial application.
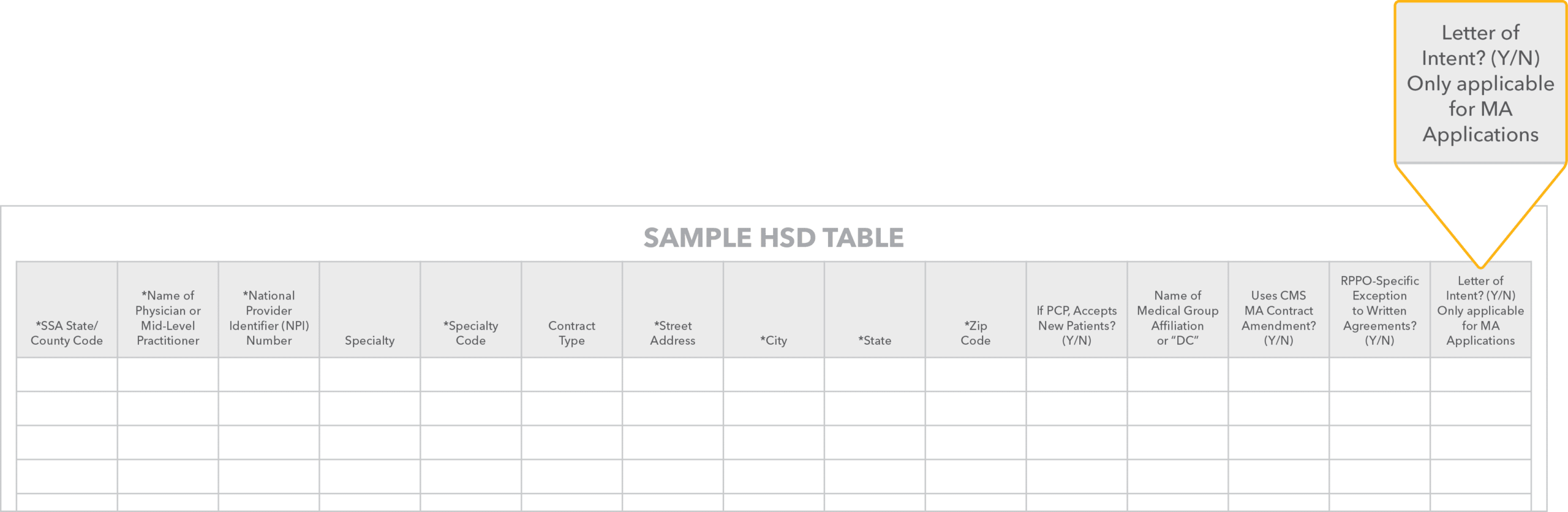
- Mark “Y” in the indicated column on the HSD table to signal intended use.
- Note that the actual Letter of Intent PDF does not need to be uploaded during the submission; however, CMS may request them anytime during or after the review process.
Tip: Use the Quest Enterprise Services®(QES®) Medicare Advantage Network Adequacy template to efficiently identify and monitor providers with a Letter of Intent in your pending counties through a dedicated column.
Q: How do applicants include Letters of Intent in their Response to Deficiency Notice and Notice of Intent to Deny?
A: When responding to the Deficiency Notice or Notice of Intent to Deny, applicants must resubmit their complete HSD tables.
Include new or additional providers or facilities with valid Letters of Intent.
Notify CMS about the use of Letters of Intent, each time they respond to any noted deficiency that they are seeking to address with a Letter of Intent.
- If an applicant needs to exclude a provider or facility for whom they no longer have a valid Letter of Intent, they must resubmit the HSD tables without that provider or facility.
- If the applicant has successfully secured a contract with the provider or facility, the applicant must remove the “Y” indicator from the Letters of Intent column.
Q: Is there a deadline for converting a Letter of Intent into a full contract?
A: Yes, all Letters of Intent must be converted into full contracts by January 1 of the go-live date to meet network adequacy requirements. Medicare Advantage Organizations must ensure that all Letters of Intent are signed into contracts before this deadline.
Q: Will an Exception Request be approved if an applicant is still in the process of contracting with a provider?
A: No, the Exception Request will not be approved in this case.
Q: What should Medicare Advantage Organizations keep in mind when using Letters of Intent?
A: Conversion into Full Contract by January 1
Letters of Intent must be fully executed contracts before January 1, of the go-live date.
Participation in the Triennial Review
If a Letter of Intent is used to secure an MA contract, that contract will be required to participate in CMS’s Triennial Network Adequacy Review during the first contract year the MA contract is operational.
Q: How can I contact CMS about Medicare Advantage and Cost Plan applications?
A: Questions regarding these updates or content related to network adequacy may be submitted to the Medicare Advantage Operations Mailbox. Select “Network Adequacy” from the category drop-down menu on the question submission page.
Please note that the guidance in this article does not apply to certain product types, including Medicare/Medicaid Plans (MMPs), section 1833 cost plans, non-network private fee-for-service (PFFS) plans, and network-based medical savings account (MSA) plans.
How does Quest Enterprise Services Solve for the Letter of Intent?
Quest Enterprise Services® (QES®) Adequacy dramatically simplifies the management of Letters of Intent. QES provides a compliant Medicare Advantage Network Adequacy template with all the necessary fields for HSD tables and Letter of Intent management, including a dedicated column that allows you to track which providers are using a Letter of Intent in your pending counties. Saving you time and effort, QES automates the entire process, eliminating the need for separate analyses or manual calculations. Manage your network with ease by scheduling a strategy session with one of our network experts to learn more.
Related Articles on Medicare Advantage Network Adequacy and Provider Directory Accuracy
Know Your Data, Grow Your Business
Get a complimentary strategy session with a Quest Analytics expert to learn how we can help you maintain network adequacy, improve data accuracy and achieve astonishing efficiencies.











