Optimize Provider Networks with Industry-Leading Provider Performance Analytics
Discover how Provider Claims Insights (PCI) empowers healthcare network strategists to enhance care quality and cost-efficiency through provider data and analytics.

QES Provider Claims Insights
Your Solution for Powerful Provider Performance Analytics
Maximize the potential of your healthcare provider networks with Quest Enterprise Services® (QES®) Provider Claims Insights (PCI). By leveraging our comprehensive claims database, which encompasses all types of payers and business lines, QES PCI provides powerful provider performance analysis. QES PCI significantly enhances provider network optimization by giving you the data you need to ensure every network decision is well-informed, each action is strategic, and every outcome is optimized for the highest standard of care.
Expand Your Network Insights
Provider Network Optimization
Efficiently address network gaps by engaging active, high-quality, cost-effective providers who are specifically proven in your line of business.
Comprehensive Data
Access our premier proprietary medical and pharmaceutical claims database, encompassing over 5 billion annual claims from Medicare, Medicaid, Veterans Affairs, TRICARE, and commercial lines of business. Elevate your network analysis with this wealth of data, outpacing internal and external sources.
Regulatory Compliance
Comply with federal and state regulations by eliminating ghost providers. Gain critical insights into provider clinical activity to distinguish active providers from inactive ones.
Revenue Optimization
Use additional cost and quality data to build and refine provider networks for cost-effective care. Advanced data insights help you reduce medical expenses and increase profitability.
- Popular Features
- Use Cases
- Related Solutions
- Related Resources
Popular Features
Discover the top features of QES PCI – your toolkit to help you better understand provider performance, enabling you to strategically build, expand, and optimize your provider networks.
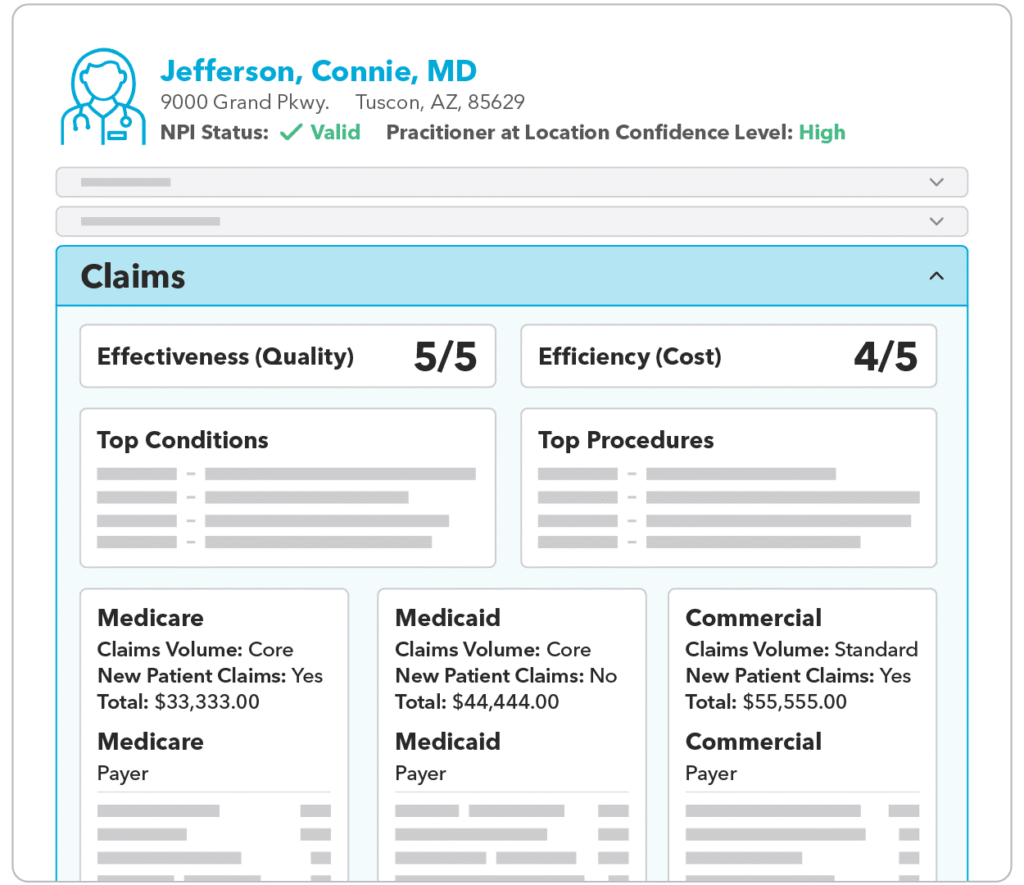
Provider Claims Data Insights
Provides unparalleled insights into provider performance and network management, leveraging our comprehensive provider claims database.
Provider Clinical Activity
Ensure regulatory compliance and prevent penalties by identifying ghost providers through provider clinical activity. Get deeper insights with total claims dollar amount and “accepting new patient” indicators segmented by line of business.
Executive Dashboard
Access intuitive dashboards for monitoring network performance across key measures, enhancing decision-making capabilities.
Provider Efficiency and Effectiveness Scores
Incorporate provider cost and quality metrics to enhance your analysis of provider network performance.
Provider Top Procedures, Conditions, and Prescribed Medications
Leverage valuable claims-based metrics, including top procedures, conditions, and medications prescribed, for a targeted approach to network performance optimization.
Practitioner At Location Confidence Analytics
Ensure accurate provider recruitment and gap-filling with additional insights within PCI for practitioners at the location.
Third-Party Data Integrations
Supplement your insights with access to premium data from trusted third-party data sources. This expanded view of provider performance indicators helps you identify top-performing providers, refine network design, and strengthen the value of your network.
New Patient Claims Indicator
Identifies if a provider has treated a new patient in the last six months, helping you think strategically about network access and supporting efforts to ensure current and new members have access to enough providers accepting new patients.
QES® Provider Claims Insights in Action
Explore how QES PCI can revolutionize your provider network management strategy, deliver measurable results, and drive success for healthcare networks nationwide.
More Efficient Gap Filling
Accelerate the closure of network gaps with actively practicing specialists, ensuring members can access the care they need.
Network Refinement
Streamline your network for peak performance, enhancing efficiency and member experiences with strategic provider alignment.

New Network Builds or Expansion
Expand your network rapidly to meet strategic goals, ensuring comprehensive coverage and member satisfaction.
Member Steerage and Referral Decision Support
Direct members to high-value care, optimizing healthcare outcomes and cost-efficiency with informed provider referrals.

Related Solutions
Enhance network performance with a powerful suite of solutions designed to seamlessly complement QES PCI. These integrated tools work together to help you build networks that are compliant, competitive, accurate, and optimized for peak performance.
Additional Data Sources
Incorporate additional data sources like Arcadia’s CareJourney and Motive Practicing Wisely to gain deeper insights into your provider data. By combining these data sets, you can uncover trends, identify opportunities for cost savings, improve provider performance, and make smarter, data-driven decisions that enhance outcomes for your members.
QES Adequacy
Integrating QES PCI data with QES Adequacy provides deeper insights to evaluate network adequacy, identify gaps, and optimize provider coverage more efficiently. This combination enhances your ability to meet compliance requirements while delivering actionable data to align your provider network with member needs. The result is improved access to care and stronger overall network performance.
QES Accuracy
Pair QES PCI with QES Accuracy to enhance provider data accuracy. With the additional data insights, you can make better-informed decisions to improve network performance and member satisfaction.
QES Competitive Insights
Leverage QES Competitive Insights in combination with QES PCI data to gain a thorough understanding of your network compared to that of your competitors. By assessing provider costs, quality, and clinical activity, you can pinpoint areas for improvement, make informed strategic decisions, and ultimately enhance provider network performance and member satisfaction.
Network Contribution
Measure your health system’s impact on payer network adequacy. Viewing your provider footprint from a payer perspective can be a valuable tool for payer negotiations or evaluating expansion opportunities.
Network Configuration
Create the optimal network by recruiting the right providers in terms of access, provider performance, competitive overlap, and other KPIs.
QES Scenario Modeling Package
Combining QES PCI with the QES Scenario Modeling Package simplifies provider network management at scale. Conduct ‘what-if’ analyses, evaluate provider changes, and leverage insights from Volume Reporting to optimize strategies and drive better outcomes efficiently.
Discover More
Dive into additional resources for more information and valuable insights.
GET STARTED WITH QES PROVIDER CLAIMS INSIGHTS
Quest Enterprise Services Provider Claims Insights helps you improve the value of your provider network by ensuring it is adequate, accurate and active! Schedule a complimentary strategy session today to learn more.

Start a Conversation Today!

















