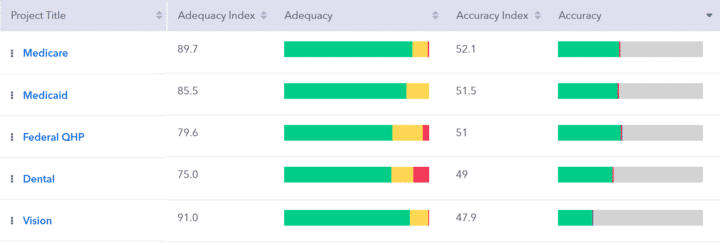
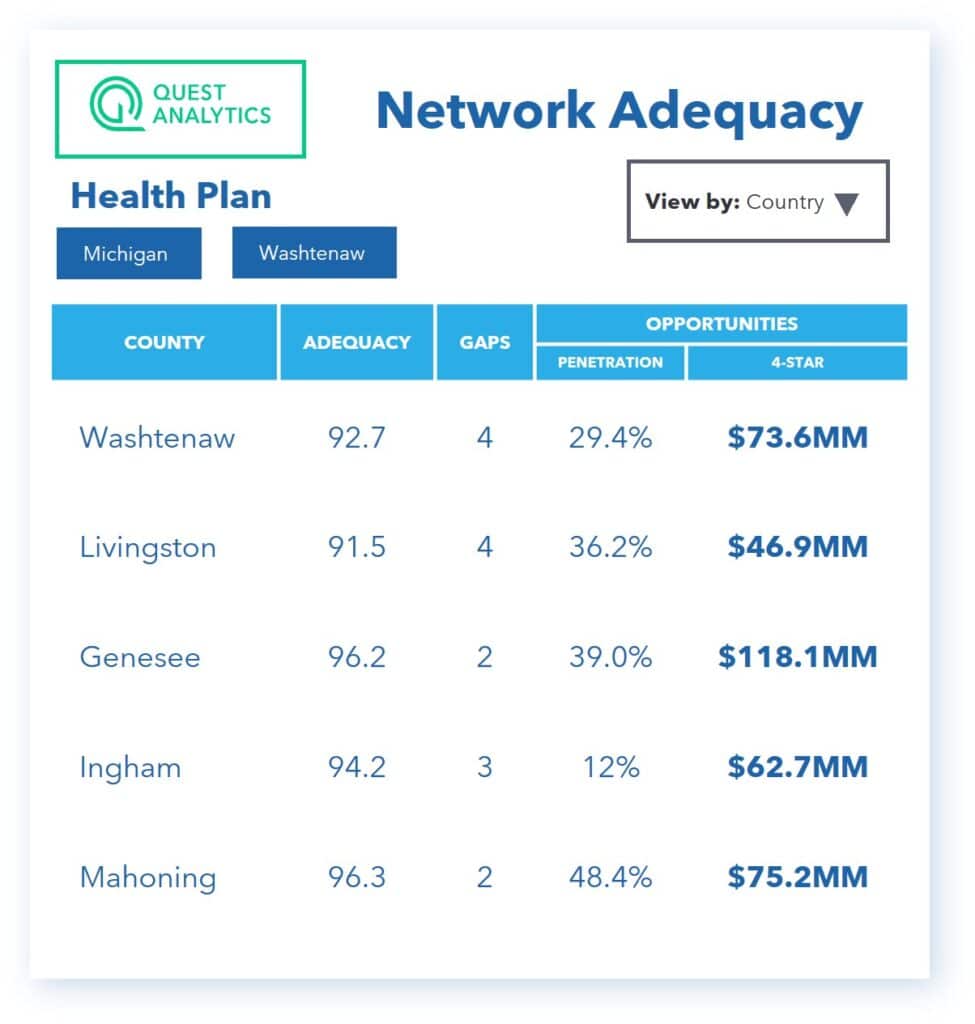
Our widely recognized pre-built Medicare Advantage Network Adequacy Template assists you in continuously evaluating your network against CMS’s standards. Designed based on federal network adequacy guidelines, these templates provide an automated solution, saving you valuable time and resources.
Provider data accuracy is paramount in assessing network adequacy and maintaining regulatory compliance. Our comprehensive provider data accuracy services offer a reliable solution for maintaining compliance and improving your provider data.