Quest Enterprise Services® (QES®)
Membership Package
Gain the Ability to Evaluate Your Network Coverage Using Two Different Membership Files Simultaneously
DUAL MEMBERSHIP Analysis: See Your Network
Analyze Network Coverage Using Two Membership Files
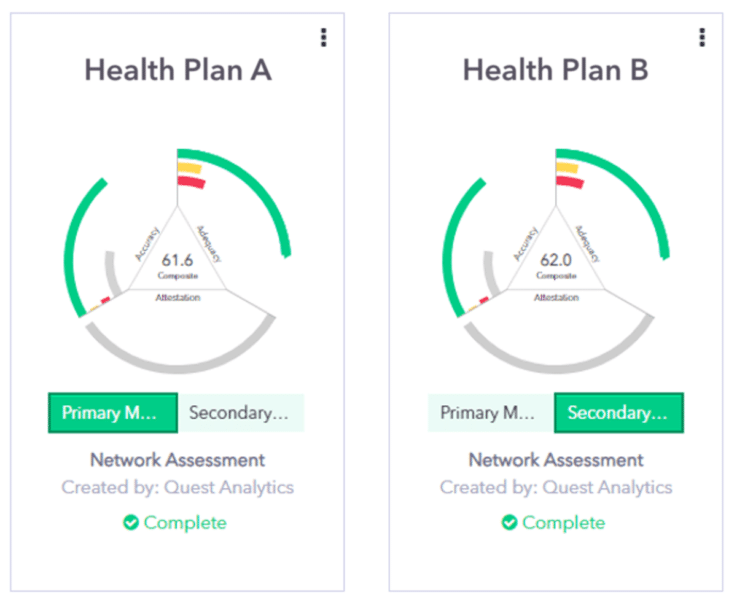
Why settle for a limited view? With our Dual Membership Analysis, you can evaluate your provider network coverage using both your membership file and the regulator-provided census file at the same time. This side-by-side capability gives you a comprehensive, 360-degree perspective of your network—allowing you to identify strengths, uncover gaps, and make data-driven decisions. Whether you’re comparing distributions or aligning with regulatory requirements, these insights save time and enhance transparency, making your analysis workflow both faster and smarter.
Membership Risk: Focus Where the Risk is Greatest
Quantify the Impact of Coverage Gaps
When a network deficiency exists, how many members does it put at risk? The Membership Risk analysis doesn’t just answer that question—it helps you take action. Visualize the exact number and percentage of members at risk of losing coverage when a gap exists, broken down by state and county views. This insight helps you prioritize filling deficiencies based on the number of members impacted. For example, if a significant portion of your members is at risk in a key area, you know where to focus your resources first. These insights are invaluable for daily management and decisions regarding Service Area Reduction or Drop County, providing clarity and confidence for your next steps.
Membership Binding: Targeted Demographic Insights
Gain Deeper Insights into Your Network Coverage
Wondering if your network meets compliance standards for specific groups? Enhance your understanding of network coverage by breaking down membership data into meaningful segments, such as age, gender, or other demographics. Focus on specific groups, like pediatric members, to evaluate coverage for particular specialties, such as Pediatric Surgery. This level of targeting enables you to assess risks with greater precision and drive actionable insights—all from one centralized location. Customize membership groups to match your unique goals, ensuring flexibility and control over every analysis.
All Your Data, Seamlessly Integrated
From Big Picture to Small Details
Bring it all together with the QES dashboard. Get a comprehensive overview or detailed views of your network:
- Analyze network coverage at multiple geographic levels.
- Configure your analysis based on actual membership or enrollee data and census files.
- Work smarter and faster with an intuitive, centralized view of your membership and risk assessments.
Discover how QES Membership Package can transform your network evaluation process
Ready to elevate your network adequacy? Schedule your Complimentary Strategy Session today and discover how the QES Membership Package can drive better data, better network management, and better member experiences. Schedule Now