The foundation of an effective provider network lies in selecting the right providers, those whose capabilities match the clinical needs of your member population. But for payers and health plans, that’s only the beginning.
Amid rising costs, shifting regulatory requirements, and growing expectations for healthcare access and quality, provider network performance management has become more complex.
Many organizations struggle with network adequacy, outdated provider data, and a lack of visibility into provider behavior and outcomes. Improving provider network performance requires a more strategic, data-driven approach, one that goes beyond compliance requirements to enable true provider network optimization. From better provider network alignment to continuous network performance improvement, here are some key steps to guide you to a high-performing network.
Establishing a Solid Foundation for Provider Network Performance
Before you make any changes, take time to establish goals, identify relevant metrics, and collaborate with your team and strategic partners. Here are three steps to get you started.
1. Set Clear Objectives
Define specific goals and timelines for your process, people, tools, and outcomes. These objectives will guide your decision-making process, whether you’re preparing for compliance requirements, an audit, expansion, or product creation.
2. Engage with Stakeholders
Involve the individuals and teams who will be impacted by the changes from the start. Their feedback, needs, and insights will help shape your strategy.
3. Evaluate the Network for Optimization and Accuracy
Conduct a thorough assessment of your provider network to understand the current status and trends. Identify any gaps or areas for improvement, such as specialties or geographical regions that lack access to care. This evaluation will serve as a baseline for refining your network effectively.
Provider Network Optimization: Factors for Selecting the Right Providers
After establishing clear objectives, it is crucial to analyze providers using metrics that align with your goals. Consider the following key factors when selecting network providers.
Network Adequacy: Does the Provider Meet Coverage Needs?
Evaluate and ensure that the providers listed in your database and directory help you comply with network adequacy standards as well as provide the necessary coverage for your membership.
While traditional standards like time, distance, and provider specialties are necessary, keep in mind that the definition of network adequacy is constantly expanding to include additional data elements. We recommend staying up to date with the latest standards and requirements for Medicare Advantage, Medicaid, and Qualified Health Plans. Regularly assess providers with updated standards to ensure the highest level of care delivery and compliance.
Provider Data Accuracy: Has the Provider Recently Verified Information?
Identify which providers have recently attested to their information, as regulations require. Providers who have not verified or updated their information should not be listed in the directory or count towards network access.
Tip: Verify provider status, specialty, contact information, cultural and linguistic capabilities, telehealth capabilities, primary office or facility address, network participation, and other required elements.
Provider Activity Levels: Is the Provider a Ghost Provider?
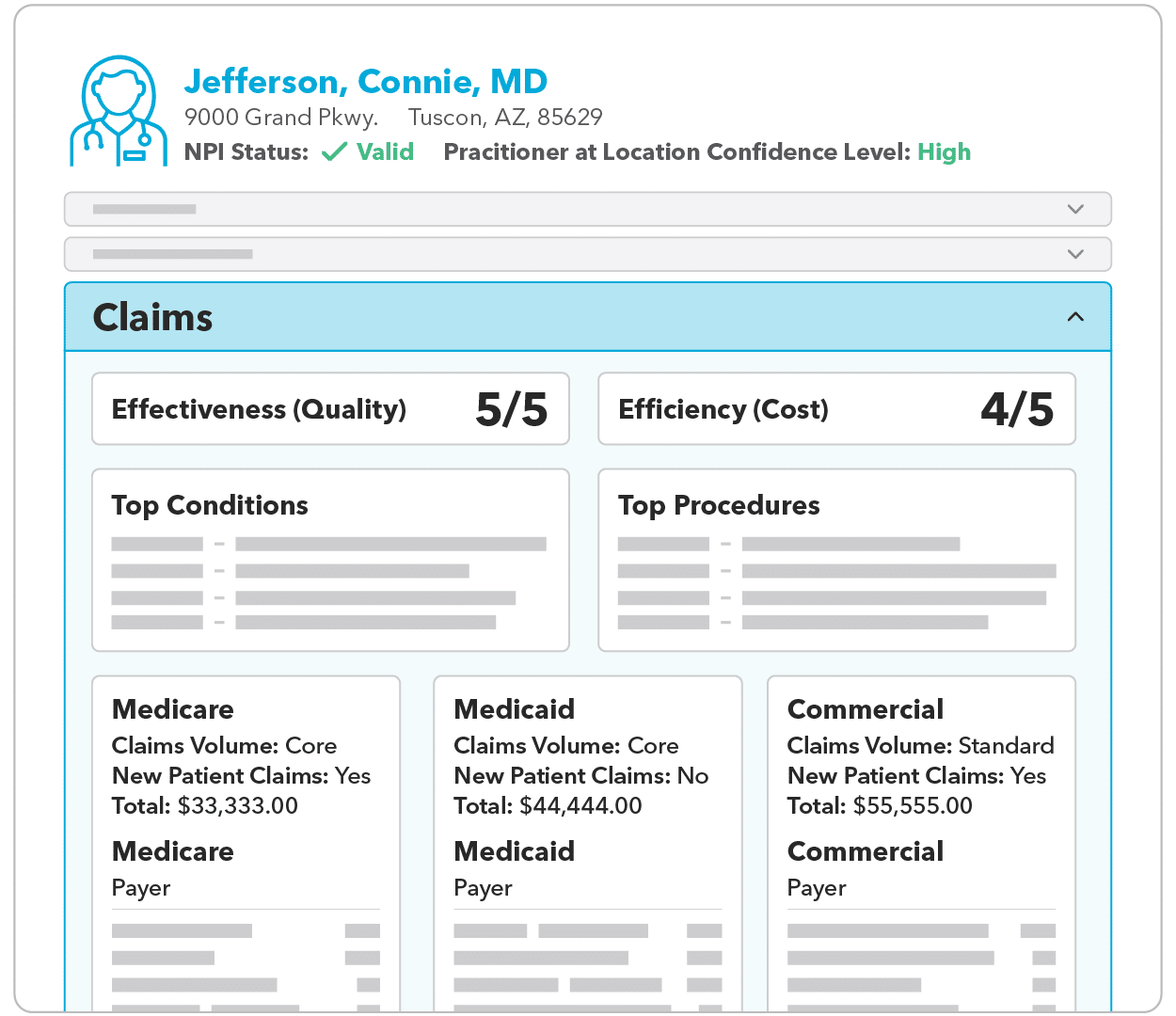
Understanding which providers are active and generating claims, and which providers are ghosts, is just as important as provider data accuracy. Having insights into each provider’s activity across different lines of business, allows you to effectively identify and differentiate between active and inactive providers.
Cost and Quality Scores: How Efficient and Effective is the Provider?
Assessing provider efficiency and effectiveness involves analyzing their cost and quality metrics. By incorporating these metrics, you can focus on the providers in your network, or those you want to add, enhance the quality of care provided, and ultimately improve patient satisfaction.
Payer Participation: Which Payer Does the Provider Work With?
Having a comprehensive understanding of each provider’s relationships with different payers allows you to optimize your network strategies and negotiate in a more efficient manner.
Conditions and Procedures: What is the Provider's Expertise?
Using data like top conditions and top procedures allows you to examine the provider’s full range of expertise beyond their general specialty. You can ensure that their expertise aligns with their actual practice, allowing for better-informed decisions when selecting providers.
Refining Provider Network Performance
Refining provider network performance is an ongoing process that requires continuous evaluation and improvement. Consider the following steps.
Identify High-Quality Providers
Get insights from your data to identify providers who align with your network objectives and have a track record of delivering top-notch care. This helps you create targeted recruitment strategies to entice those providers and negotiate contracts that boost performance.
Collaborate Across Teams
Consider using an enterprise provider network management solution such as Quest Enterprise Services® to enhance collaboration among teams. This solution enables teams to conduct “what-if” scenarios and effectively share provider and network analytics. By allowing all teams to access the same data insights, it improves discussions, aligns activities with organizational goals, and promotes continuous improvement.
Continuous Monitoring and Adjustment
Regularly monitor key metrics, reassess network adequacy, and make adjustments as needed to meet changing member needs and adapt to market demands.
Turning Strategy into Sustained Provider Network Performance
Improving provider network performance is an ongoing effort that goes far beyond initial provider selection. It requires a strong foundation, continuous refinement, and a commitment to aligning your network with the evolving needs of your member population. By carefully selecting the right providers, monitoring network adequacy, and leveraging data to drive provider network optimization, you can enhance both the quality of care and member experience.
As regulatory pressures increase and expectations for access, transparency, and outcomes grow, organizations that invest in proven provider network performance management will be best positioned for success. From physician network optimization to continuous performance improvement, building a smarter, more resilient provider network starts with the decisions you make.
Proven Solutions for Your Provider Network Management
Looking to simplify your workload? Let Quest Analytics take on the heavy lifting! Our solutions and dedicated team specialize in provider data accuracy and provider network adequacy for various lines of businesses, including Medicare Advantage, Medicaid and Commercial. Schedule a strategy session today and see how we can help you every step of the way.