Quest Enterprise Services® (QES®)
Advanced Decision Applications
Power Up Your Provider Network Adequacy Management
Discover innovative tools that provide exceptional data insights and boost productivity, empowering you to reduce network adequacy compliance risks, and make strategic decisions with confidence.

Quest Enterprise Services® Advanced Decision Applications
Your solution for unparalleled network insights and productivity
The Advanced Decision Applications suite in Quest Enterprise Services® (QES®) is here to make provider network management simpler and more efficient. With tools dedicated to scenario modeling, handling network adequacy exceptions and justifications, and advanced membership analysis, your team can address business needs effectively.

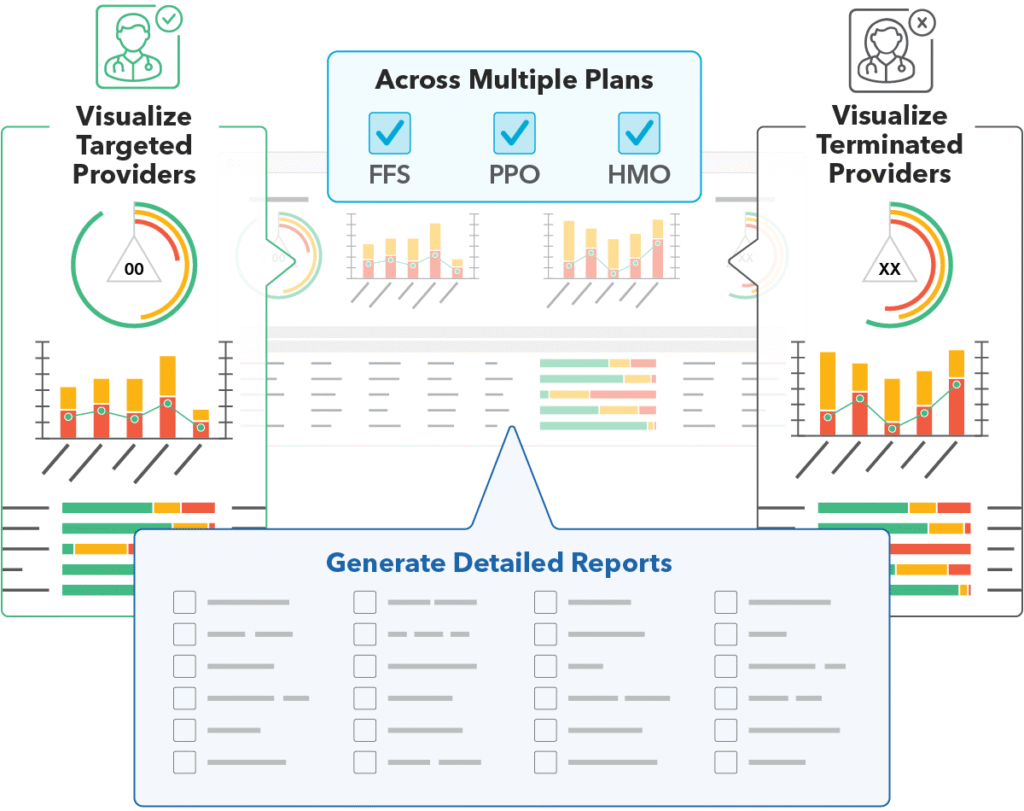
Quest Enterprise Services Scenario Modeling for Provider Data Management at Scale
Quest Enterprise Services Enterprise Compliance Dashboard for Enhanced Network Visibility
- Gain Multiple Perspectives: View your network by county, line of business, specialty, and exceptions.
- Pinpoint Network Adequacy Needs: Identify gaps, network changes, exclusions, and exceptions across all lines of business.
- Streamline Workflows: Reduce time and resources spent on external dashboards and redundant tasks.
- Enhance Decision-Making: Use sophisticated visualizations to elevate and expedite leadership actions.
Quest Enterprise Services Network Adequacy Exceptions
- Exception Request Document Generator: Effortlessly generate CMS Medicare Advantage (MA) and Medicare-Medicaid Plan (MMP) Network Adequacy Exception Request documents using your QES Adequacy Exception inputs.
- Pattern of Care Providers: Efficiently add providers to Health Service Delivery (HSD) tables for CMS submissions to support exception narratives.
- Zip Code Summaries: Easily identify members who don’t have access to care within the regulatory standard at a zip code level.
- Next Closest Network Provider: Quickly find the distance or time to the next closest network provider.
- Next Closest Market or Prospect Provider: Identify the next closest Market or Prospect Provider between members that do not have access and the Next Closest Network Provider within the established standard to provide for exception requests.
- Verified Sources: Utilize the populated list within QES to easily select your sources from a drop-down list and export it for the required form.
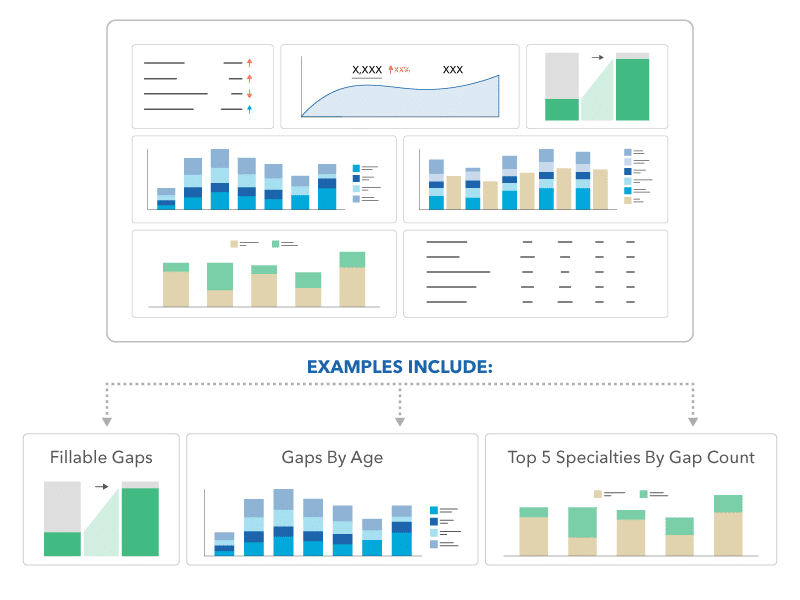
Quest Enterprise Services Membership Analysis
- Membership Analysis – Run analyses based on your custom membership distribution file.
- Membership Compare – Compare analyses across membership distribution data or with the sample beneficiary file.
- Membership Risk – See the number of members at risk due to any deficiencies, or gaps, in your provider network at the state and county levels.
- Membership Binding – Assign a specific subset of your membership to a given specialty.
Discover More
Dive into additional resources for more information and valuable insights.
Ready to Elevate Your Network Management?
Discover how Quest Enterprise Services can transform your provider network management and elevate your operational efficiency. Connect with us today to get started.

Start a Conversation Today!